As healthcare leaders, we’re united by a common goal of improving patient outcomes. We invest in advanced diagnostics, cutting-edge treatments, and talented clinical teams. Yet, we often find the most significant barriers to health exist outside our clinics and hospitals.
These powerful, non-medical factors are known as the Social Determinants of Health (SDoH). Understanding and addressing these factors is a matter of public health and an important business strategy for health plans, hospital systems, and large provider groups.
What Are The Social Determinants of Health?
Social determinants of health are the conditions in which people are born, grow, live, work, and age. These factors are the fundamental drivers of health inequities and outcomes.
Effectively managing social determinants of health can lead to lower costs, improved quality metrics, and a more sustainable healthcare ecosystem.
The 5 Social Determinants of Health
To effectively address SDoH, we must first understand its core components. The U.S. Department of Health and Human Services organizes these factors into five key domains. It’s important to understand the challenges in each of the specific social determinants of health examples within this framework to see the whole picture.
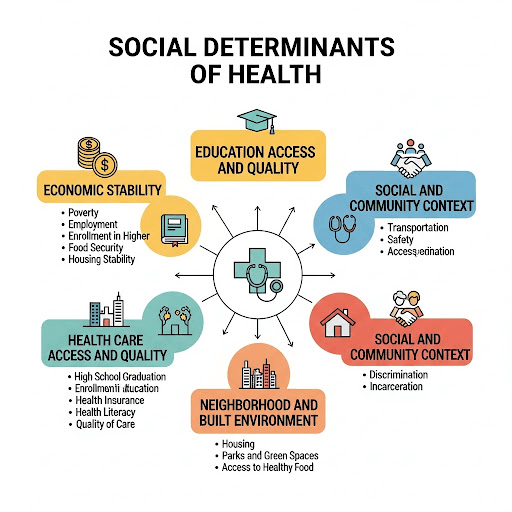
1. Economic Stability
This domain encompasses a person’s ability to meet their basic needs. When a patient is financially unstable, their health is often the first thing to be compromised.
Key Factors
- Poverty
- Employment status
- Food security
- Housing stability
Real-World Example
Consider a single parent working a low-wage job without paid sick leave. The constant stress of choosing between paying rent, buying groceries, or affording their child’s asthma medication can lead to chronic stress, elevating cortisol levels, and increasing the risk of hypertension and heart disease.
They might miss preventative care appointments because they can’t afford the co-pay or the time off work, which can turn a manageable condition into a costly health crisis.
2. Education Access and Quality
Education is a powerful predictor of long-term health. It equips people with the skills for better jobs and the knowledge to make healthier choices.
Key Factors
- Early childhood development
- Enrollment in higher education
- Language and literacy
- Health literacy
Real-World Example
A lack of quality education earlier in life often reduces the likelihood of attaining higher education, leading to fewer stable job opportunities and, consequently, lower lifetime income. This economic strain is one part of the problem. The other is that the same educational gap often results in lower health literacy.
Imagine an elderly patient recently diagnosed with diabetes. They may struggle to understand complex instructions about blood sugar monitoring, insulin administration, or dietary changes. This confusion can lead to poor glycemic control, frequent hospitalizations, and preventable complications like neuropathy or vision loss.
In this way, an educational deficit from decades prior impacts not only their financial well-being but also their fundamental ability to manage their health.
3. Health Care Access and Quality
This domain is where we have the most direct influence, yet significant barriers remain.
Key Factors
- Insurance coverage
- Access to primary care
- Transportation to services
- Provider availability
Real-World Example
Think about a person living in a rural community. The nearest specialist might be a two-hour drive away, and public transportation is nonexistent. This lack of transportation is a significant barrier. They may delay or forgo necessary screenings, like mammograms or colonoscopies, simply because they can’t physically get to an appointment.
This directly increases their risk of a late-stage cancer diagnosis, where treatment is less effective and far more costly for the health system.
4. Neighborhood and Built Environment
Our physical environment plays a massive role in our daily health. Safety, access, and exposure to toxins can either support well-being or undermine it.
Key Factors
- Access to healthy foods
- Quality of housing
- Crime and violence
- Environmental conditions
Real-World Example
Let’s look at a family living in an urban neighborhood with high rates of crime and violence and no safe parks. Children may be forced to stay indoors, leading to a sedentary lifestyle and a higher risk of obesity and diabetes. Furthermore, if their apartment has issues such as mold or pest infestations, these can trigger asthma and other chronic respiratory illnesses, leading to repeated emergency room visits.
5. Social and Community Context
This domain refers to the relationships and social networks that create a sense of belonging and support.
Key Factors
- Social cohesion
- Civic participation
- Experiences with discrimination
- Incarceration history
- Support system
Real-World Example
Consider someone who is part of a marginalized community and regularly experiences discrimination. This can lead to chronic stress and a deep-seated mistrust of the healthcare system, causing them to avoid seeking care until a problem becomes severe. A lack of strong social support systems can also exacerbate feelings of loneliness and isolation, which studies have linked to a higher risk of depression, cognitive decline, and even mortality.
The Strategic Imperative of SDoH Screening
Identifying these barriers is the first and most critical step. This is where SDoH screening programs become essential. A well-designed social determinants of health screening tool is a vital data-gathering instrument that uncovers the root causes of poor health outcomes.
However, implementing an effective SDoH screening tool presents significant challenges. The process can be resource-intensive, requiring dedicated staff, patient outreach, and a data management system. Furthermore, screening alone is not enough. Simply identifying a need without a straightforward way to connect the patient to a solution can lead to frustration and further disengagement. We must have the infrastructure in place to act on the information we gather.
The Aeroflow SDoH Program
Recognizing this immense challenge, Aeroflow Health developed a comprehensive solution. The AeroflowSDoH Program is designed to partner with health plans and providers to bridge the gap between identifying social needs and connecting patients to the resources they need.
Our program addresses the key domains of SDoH by:
- Simplifying Access: We manage the entire enrollment and verification process, helping patients and caregivers access essential services like health insurance, nutrition assistance (SNAP), and housing support.
- Providing Expert Navigation: Our team of dedicated specialists understands the complexities of social service systems. We offer both digital and direct verbal support to guide patients and caregivers to the resources they need.
- Creating a Data-Driven Partnership: We provide our partners with clear data and insights, helping you understand the specific needs of your patient population and track the impact of our interventions.
We understand your primary focus is delivering quality medical care. Our program acts as a direct extension of your team, managing the complex, non-medical barriers that are so critical to patient success. We handle the logistics of social support so you can focus on what you do best.
Learn more about partnering with the Aeroflow SDoH Program.
Are you a health plan interested in learning more about our SDoH program? Contact us here.